Ingredients
- What is Mediastinum? Mediastinum Region and Anatomical Significance
- What are Mediastinal Masses and Tumors?
- Anterior Mediastinal Masses (Thymoma, Teratoma, Lymphoma)
- Middle and Posterior Mediastinal Tumors (Neurogenic Tumors and Cysts)
- Thymus Gland Diseases and Thymoma
- What is Thymoma? Symptoms and Stages
- The Relationship Between Myasthenia Gravis and the Thymus Gland
- Symptoms and Clinical Findings in Mediastinal Tumors
- Diagnosis and Diagnostic Methods
- Computed Tomography (CT) and MRI Examinations
- Biopsy with Mediastinoscopy and EBUS
- Mediastinum and Thymus Surgery Methods
- Closed Thymus Surgery (VATS and Robotic Surgery)
- Thymectomy (Thymus Gland Removal) Surgery
- Mediastinal Mass Extirpation (Open and Closed Techniques)
- Postoperative Recovery Process and Follow-up
- Frequently Asked Questions
- Is Mediastinal Surgery Risky?
- Does the Disease Recur After Thymoma Surgery?
- How Much Do Myasthenia Gravis Patients Benefit from Surgery?
Mediastinum and thymus surgery encompasses specialized operations of a critical area located in the very center of the chest cavity and home to vital organs.
This region is between both lungs; It is a narrow but extremely complex space that houses the heart, major vessels, esophagus, and trachea.
Mediastinal surgery utilizes the most advanced techniques of modern thoracic surgery in treating both benign cysts and malignant tumors.
Today, these surgical interventions are performed with closed methods instead of large incisions thanks to developing technology, optimizing the patient’s recovery process.
What is Mediastinum? Mediastinum Region and Anatomical Significance
Mediastinum is the name given to the anatomical space between the right and left lungs in the rib cage.
This area, which is bounded by the sternum in the front and the spine in the back, is like the traffic center of the body.
The main vessels coming out of the heart (such as the aorta), the main airways, the esophagus and the lymph nodes are in very close neighborhoods to each other in this narrow area.
Due to this anatomical compression, even a small mass that develops in the mediastinum area can put pressure on vital organs, leading to serious symptoms.
Surgeons use the mediastinum to better analyze this area; They divide it into three virtual regions: anterior, middle and posterior mediastinum.
What are Mediastinal Masses and Tumors?
Masses seen in the mediastinum originate from cells with different characteristics according to their location.
Some of these masses are congenital cysts, while others are tumors originating from gland tissues or nerve sheaths.
Anterior Mediastinal Masses (Thymoma, Teratoma, Lymphoma)
The anterior mediastinum is the area located just behind the breastbone and is the most common area where masses are seen.
- Thymoma: It is the most common anterior mediastinal tumor originating from the thymus gland.
- Teratoma: They are germ cell tumors that are common in young adults and can contain different types of tissues (hair, teeth, etc.).
- Lymphoma: They are masses that originate from the lymphatic system and usually require systemic treatment (chemotherapy).
- Thyroid Appendages: The growth of the goiter in the neck into the rib cage (plonjan goiter) can be observed as a mass in this area.
Middle and Posterior Mediastinal Tumors (Neurogenic Tumors and Cysts)
The middle mediastinum usually houses lymph nodes and congenital bronchogenic or pericardial cysts.
The posterior mediastinum is the main center of “neurogenic tumors” originating from the nerve tissues in the anterior part of the spine.
Although these tumors are generally benign, they require technically precise surgical planning due to their proximity to the spinal canal.
Thymus Gland Diseases and Thymoma
The thymus gland is an organ that plays a role in the development of the immune system and is active in childhood and shrinks in adulthood.
However, in some individuals, this gland may enlarge (hyperplasia) instead of shrinking or tumoral structures may develop on it.
What is Thymoma? Symptoms and Stages
Thymoma is a tumor that originates from the epithelial cells of the thymus gland and is usually detected between the ages of 40-60.
Although the tumor tends to grow slowly, it has the potential to invade the surrounding tissues (pleura, vessels).
Staging is done according to the degree to which the tumor has exceeded its capsule; While surgery alone is sufficient in the early stages, radiotherapy support may be required in advanced stages.
The Relationship Between Myasthenia Gravis and the Thymus Gland
Myasthenia Gravis (MG) is a neurological disease characterized by fatigue and weakness in the muscles.
Approximately 15% of MG patients have a thymoma focus, while 30-45% of patients with thymoma have Myasthenia Gravis symptoms.
Surgical removal of the thymus gland (thymectomy) plays a critical role in reducing drug dependence and controlling disease symptoms in MG patients.
Symptoms and Clinical Findings in Mediastinal Tumors
Most of the masses are detected incidentally on lung x-rays taken for another reason.
However, when the mass reaches a certain size or presses on surrounding tissues, the following symptoms are observed:
- Breast Pain and Feeling of Fullness: A blunt pain felt behind the breastbone.
- Cough and Shortness of Breath: It occurs as a result of pressure on the trachea.
- Difficulty Swallowing: Compression of the esophagus by the mass from the outside.
- Hoarseness: The nerve going to the vocal cords is affected by the mass.
- Vena Cava Superior Syndrome: Swelling in the face and arms due to pressure on the main vein, prominence in the veins.
Diagnosis and Diagnostic Methods
Modern diagnostic methods clearly reveal not only the location of the mass, but also its character and its relationship with the surrounding vessels.
Computed Tomography (CT) and MRI Examinations
Medicated (contrast) Chest Tomography is the most basic and indispensable diagnostic tool for mediastinal masses.
MRI (Magnetic Resonance), on the other hand, provides superiority in determining the relationship of nerve-derived tumors, especially in the posterior mediastinum, with the spinal cord.
Biopsy with Mediastinoscopy and EBUS
Tissue diagnosis may be required to understand the character of the mass and to stage it before surgery.
“Mediastinoscopy” or bronchoscopic ultrasonography (EBUS), which is entered through a small incision in the neck, determines whether the treatment will be surgical or oncological by taking a biopsy of the lymph nodes.
Prof. Dr. Levent Alpay: The key to success in mediastinal surgery is “anatomical dominance” and “technological adaptation”. The lesions in this area are in millimeter proximity to the heart and main vessels. Therefore, our priority is not only to remove the mass, but also to preserve these vital structures and ensure the patient’s neurological comfort after surgery.
Mediastinum and Thymus Surgery Methods
These surgeries, which used to require cutting the sternum from one end to the length (sternotomy), are now performed with minimally invasive techniques.
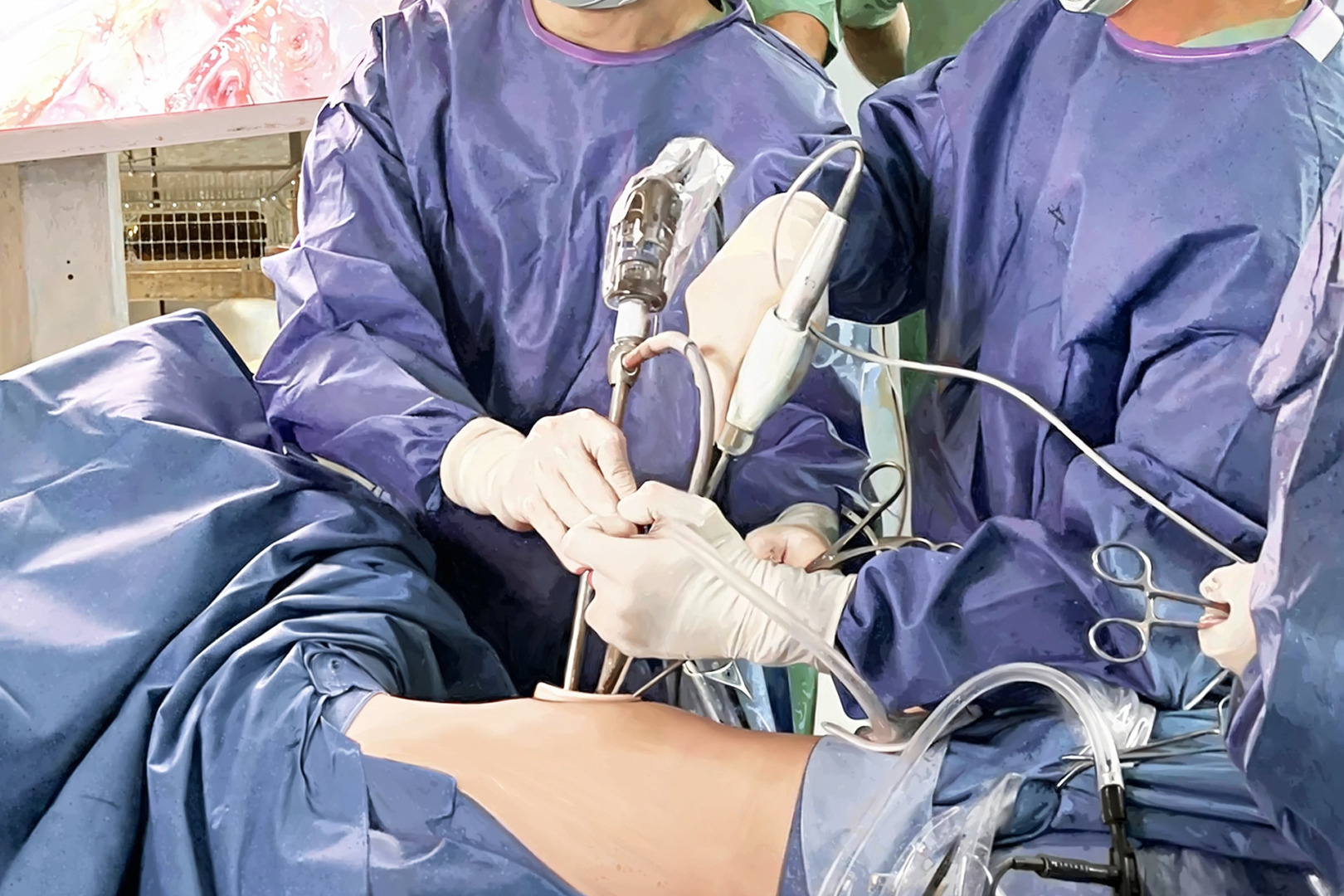
Closed Thymus Surgery (VATS and Robotic Surgery)
Video-Assisted Thoracoscopic Surgery (VATS) is performed with 1-3 small holes drilled from the side of the rib cage.
The wide image taken with the help of the camera allows the surgeon to meticulously clean the thymus gland and surrounding fatty tissues.
Robotic surgery, on the other hand, provides a high level of success in mediastinal masses with its high maneuverability in narrow spaces.
Thymectomy (Thymus Gland Removal) Surgery
It is the process of completely removing the thymus gland, especially in patients diagnosed with Myasthenia Gravis or Thymoma.
Simply removing the tumor is not enough; In order to prevent the risk of recurrence, all “peritimic” fat tissues must be removed (maximal thymectomy).
Mediastinal Mass Extirpation (Open and Closed Techniques)
Open surgery (sternotomy or thoracotomy) may still be required for very large masses or tumors surrounding the main vessels.
However, in most cases saved by surgical margins, closed techniques are considered the “gold standard”.
Mediastinal Surgery Methods vs. Recovery
| Feature | Closed Method (VATS/Robotics) | Open Method (Sternotomy) |
| Incision Size | 1 – 2 cm (3 pieces) | 15 – 20 cm |
| Hospital Stay | 2 – 3 Days | 5 – 7 Days |
| Pain Level | Minimum | Moderate / Severe |
| Return to Normal Life | 1 – 2 Weeks | 4 – 6 Weeks |
Postoperative Recovery Process and Follow-up
Patients who undergo surgery with the closed method usually start walking and eating normally the day after the operation.
The chest tube is usually withdrawn within 24-48 hours and the patient is discharged in a short time.
In thymoma cases, regular tomography checks and, if necessary, oncological follow-ups are planned according to the pathological stage of the mass.
Case Experience (Anonymous):
In a 32-year-old female patient with complaints of drooping eyelids and arm weakness (Myasthenia Gravis), 3 cm thymus enlargement was detected on tomography. Closed (Uniportal VATS) thymectomy was performed through a single hole. In the 1st postoperative year, the patient’s need for medication decreased by 70% and his neurological findings stabilized.
For detailed information about the surgical treatment of mediastinal masses and thymus diseases, you can seek expert opinion and make an appointment with our clinic.
Frequently Asked Questions
Is Mediastinal Surgery Risky?
Although every surgical procedure has general risks, vital complication rates are very low thanks to modern closed techniques and anesthesia methods.
Does the Disease Recur After Thymoma Surgery?
The risk of recurrence is very low in early-stage thymomas that are completely removed; However, it is an oncological rule to follow the patient radiologically for many years.
How Much Do Myasthenia Gravis Patients Benefit from Surgery?
After thymectomy, most patients experience a significant reduction in complaints; Full recovery or transition to a drug-free period may vary from patient to patient and the duration of the disease.
Scientific Bibliography
- Journal of Thoracic Oncology: Masaoka-Koga staging system and ITMIG recommendations
- The Annals of Thoracic Surgery: VATS Thymectomy for Myasthenia Gravis
- PubMed: Outcomes of robotic-assisted mediastinal mass resection
- Lancet Neurology: Thymectomy in Myasthenia Gravis: Clinical Trials